Electromyography (EMG) testing is a valuable diagnostic tool used to assess the health of muscles and the nerve cells that control them. By measuring the electrical activity of muscles at rest and during contraction, clinicians can gain insights into neuromuscular disorders, helping to pinpoint conditions such as carpal tunnel syndrome, peripheral neuropathy, and muscular dystrophies. As the prevalence of these disorders continues to rise, understanding the significance and methodology of EMG testing becomes increasingly essential for both healthcare providers and patients.
This article delves into the process of EMG testing, detailing its indications, what patients can expect during the procedure, and how to interpret the results. With advancements in technology and a growing emphasis on accurate diagnostics, EMG testing remains a cornerstone in neurology and rehabilitation, paving the way for effective management and treatment plans tailored to individual needs.
Understanding the EMG Procedure
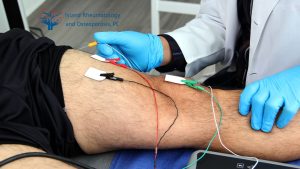
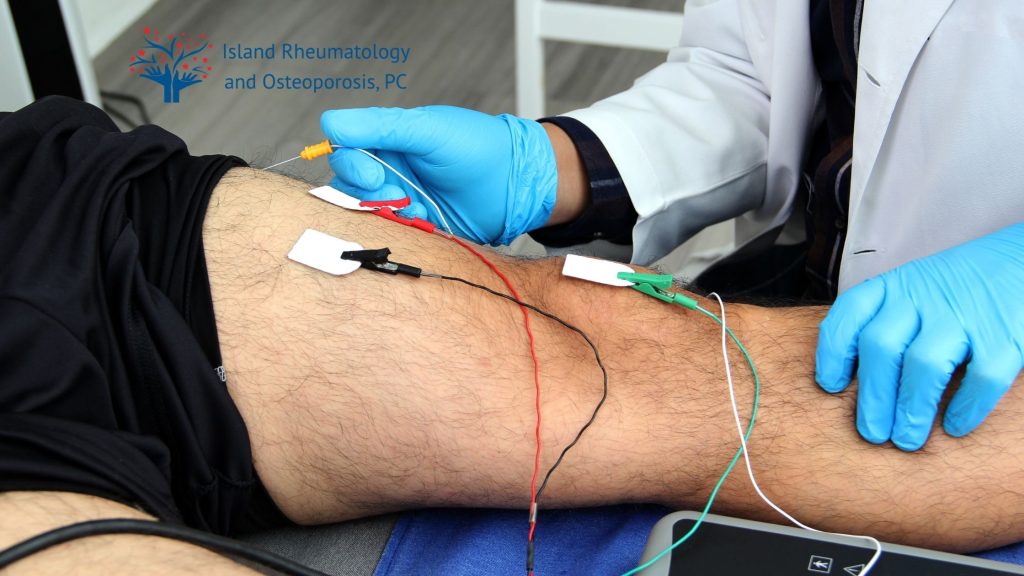
During an EMG test, small electrodes are placed on the skin over the muscles being examined. In some cases, a fine needle electrode may be inserted directly into the muscle to provide more precise readings of electrical activity. Patients may experience mild discomfort during this process, but it is generally quick and informative. The test can help identify the presence of nerve or muscle damage by evaluating the electrical signals generated during both rest and contraction. As patients prepare for their EMG, it is important to discuss any medications or medical conditions with their healthcare provider, as these factors can influence the results of the test. Understanding these elements can help alleviate anxiety and ensures that the emg testing is as effective as possible.
Interpreting EMG Results
Once the EMG procedure is complete, the collected data is analyzed by a neurologist or other trained specialist. Results are interpreted in conjunction with clinical findings and other diagnostic tests to arrive at a comprehensive diagnosis. Variances in electrical activity may indicate specific neuromuscular disorders and help differentiate between muscle diseases and nerve disorders, which is crucial for establishing an appropriate treatment plan. By accurately interpreting EMG results, healthcare providers can recommend targeted therapies, rehabilitation strategies, or further diagnostic testing, ultimately contributing to improved patient outcomes.
In conclusion, EMG testing serves as a critical element in the diagnostic landscape of neuromuscular health, providing valuable insights that guide clinical decision-making. By effectively assessing the electrical activity of muscles and nerves, this non-invasive procedure helps to unveil the underlying causes of various ailments, facilitating timely and appropriate interventions. As both technology and our understanding of neuromuscular disorders evolve, the role of EMG testing is likely to expand, ensuring that patients receive tailored and effective care. Through clear communication between patients and healthcare providers about the procedure and its implications, EMG testing not only enhances diagnostic accuracy but also empowers patients to take an active role in their treatment journey.